WHY CAN’T MY CHILD SLEEP?

This article was published in the Autism Eye Magazine. Written by Stella Chadwick BSc (hons) mBANT, CNHC
It is estimated that between 50% to 80% of children with ASD have sleep issues. In this article, I will consider the underlying contributory factors to poor sleep and will assess environmental, medical and nutritional influences. Sleep disturbance has been shown to impact concentration, mood, memory recall, and sensory processing systems. These are common issues affecting many of the children we see in our clinics.
Creating the right sleep environment
It’s important to ensure that the place your child sleeps is conducive to sleep with adequate darkness. Even the slightest ray of light can inhibit the production of melatonin (sleep hormone).
Studies by Harvard Medical School have shown that the blue light emitted from computers and mobile devices are very disruptive at night and significantly affect the production of melatonin. It is their recommendation that all devices are switched off at least 2 hours before bed.
Ensuring adequate daily exercise has been shown to not only to help children fall asleep more easily but also for them to experience deeper sleep. Some children have outgrown naps but continue to have them which may have a knock-on effect on their nighttime sleep. Is your child ready to stop daytime naps?
Could it be medical?
According to a number of estimates prevalence of seizures in those with ASD is between 11% and 39% with more than 20% of seizures estimated to occur during sleep. If you suspect this then have it investigated by your medical team.
Silent reflux can also be a major problem especially in those with a history of antibiotic use as well as other medication. If you notice bits of food in the stool regularly or lots of burping after meals and your child is not thriving physically then consider this as something to flag to your medical team.
A 2017 study by a group of Japanese researchers from Osaka University found that correcting obstructive sleep apnea had a significant impact on the behaviour of children with ASD. There is a strong link between sleep apnea and low iron levels which is extremely common in ASD children. Discuss this with your GP.
The impact of food on sleep:
Blood sugar levels
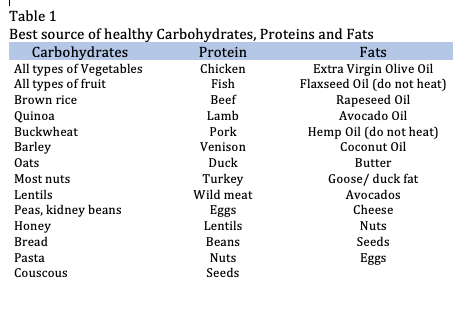
In terms of diet, the most significant thing to get right is to ensure that your child has balanced blood sugar levels. Too many carbohydrate-rich foods loaded with sugar are likely to cause huge spikes in blood sugar levels followed by a big crash. Often kids become agitated, hyper, lose focus and find it extremely hard to unwind and sleep. Ensure a balance of proteins, healthy fats, and unprocessed carbohydrates. See Table 1 below for healthy options.
Food intolerances
Food intolerance is one of the biggest culprits when it comes to poor sleep with the most common offenders being an intolerance to: gluten, dairy, corn, soy and eggs as well as some nuts. This is crucial to have assessed and addressed.
Histamine levels
Children with high histamine levels are also amongst some of the poorest sleepers. Histamine levels normally drop at night but in a body that has problems regulating histamine, the level stays high. One of the mechanisms for the body to lower histamine is to release adrenaline which of course gives energy to the system so kids become hyper. Lowering histamine level through diet and targeted supplements including enzymes can be significant for a child. (I wrote a detailed article on High Histamine Levels you may be interested in here.)
Phenols (food colouring)
Phenols are healthy compounds that give colour to plant foods and have been hailed as top anti-oxidants in protecting our cells. There are also man-made ones found in food colouring. There are a group of kids who are not very good at processing phenols. High levels of unprocessed phenol can cause hyperactivity and major sleep disturbances. If your child gets really hyper with food containing artificial colouring or is addicted to berries, apples, bananas, raisins, and dairy produce for example, then consider phenol issues. See Table 2 below for typical symptoms of those with phenol sensitivity.
Glutamate
Foods high in free glutamate can be found in abundance in almost all processed foods. They are also found in high levels in some natural foods such as tomatoes and parmesan cheese as well as bone broth. Glutamate is an excitatory neurotransmitter and works along with GABA, our calming neurotransmitter, which is essential for speech. Too much glutamate can cause significant hyperactivity and behavioural issues and sleep disturbances. www.unblindmymind.org has further information.
Which supplements are helpful?
Addressing environmental and medical issues as well making the right dietary changes can in many cases have a significant positive impact. Sometimes, however, we need more, and this is when certain supplements can be helpful. The precursor to melatonin is serotonin which is a feel-good neurotransmitter.
Those with low serotonin are generally the kids who are anxious, irritable, and prone to OCD and aggression. Using supplements like Tryptophan, 5-HTP, vitamin B6, zinc, magnesium, and Vitamin C, have all been shown to enhance this conversion from serotonin to melatonin and induce sleep. 98% of serotonin is made in the gut and not the brain so kids with low levels need lots of gut support.
If your child, on the other hand, is lethargic, doesn’t really have any interests or can’t be bothered with much and tends to be prone to anxiety then looking at improving dopamine levels might be preferable. Dopamine is another key neurotransmitter often out of balance in ASD. Supplements such as tyrosine, curcumin, gingko biloba as well as L-theanine can be really helpful. Gut-support is also key.
Taurine is an amino acid, good at calming down the nervous system and helping promote sleep. It’s highly concentrated in the brain and is significant in helping keep the balance of magnesium and calcium as well as sodium and potassium in our cells. Those following a vegetarian diet and those prone to constipation or pale/yellow/orange stools may benefit with supplementation.
Conclusion
As ever it is important to look for the underlying contributory factors to any symptom and work to resolve the root of the problem for long lasting results.
Disclaimer: This article is for educational purposes only and any changes to diet or the addition of any supplements must be discussed with your practitioner and medical professional.