WHAT’S LYME GOT TO DO WITH IT?
Featured article in the Autism Eye magazine. Written by Stella Chadwick.
Over the last decade two conditions have increased to near epidemic proportions. The first is autism. The second is Lyme disease.
Lyme disease is one of the most misunderstood diseases of our time. It is not a new disease, but it is controversial, and does not discriminate who it infects, with some evidence that children between the ages of 5 and 9 are particularly at risk. It is estimated that more children are diagnosed with Lyme disease each year than all the cases of epilepsy, type 1 diabetes, cystic fibrosis and paediatric cancer combined.
Whilst correlation does not always mean causation, according to DR Klinghardt, a key authority on Lyme disease, over 70% of the children he has seen with neurodevelopmental disorders have tested positive for Lyme disease. Furthermore, 84% of the mothers of children with autism have also tested positive for Lyme disease.
What is Lyme Disease?
Lyme disease is generally known to be caused by the Borrelia burgdorferi bacteria, which has become known as the super-microbe. Borrelia is clever enough to hide in the host’s own blood cells and body tissue to evade the immune system. It has the ability to suppress the immune system and survive in the most hostile of environments.
There are a number of species and over 300 different strains of Borrelia worldwide, making Lyme disease one of the most challenging diseases to diagnose. Even the best laboratories are limited to the number of species and strains that they test for. Each strain can cause slightly different symptoms and immune reaction. In Europe, for instance, Borrelia afzelii can cause skin rashes and Borellia garinii can cause neuroborreliosis, which affects the central nervous system.
How is Lyme disease transmitted?
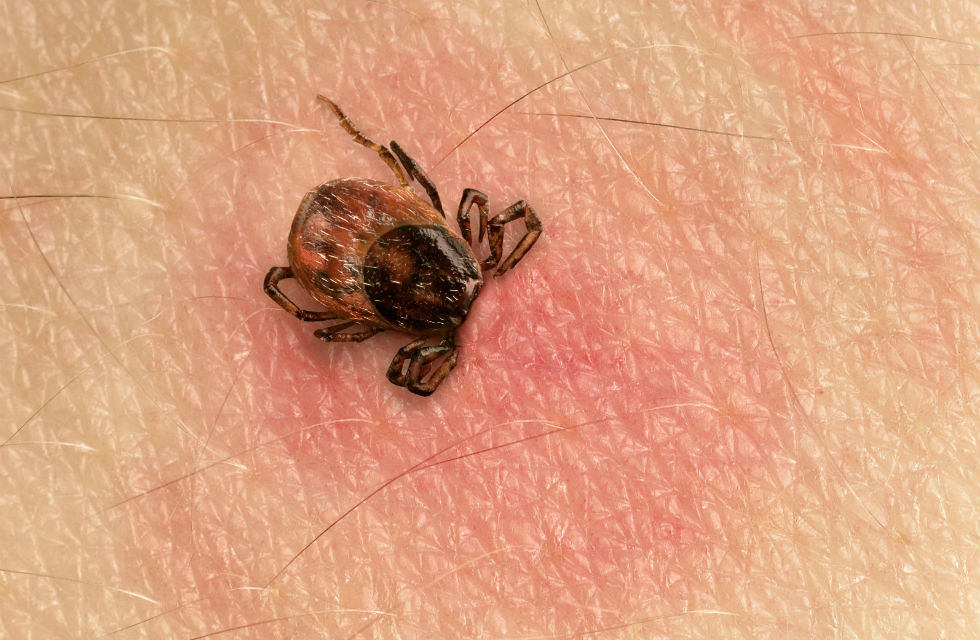
The traditional idea that Lyme disease can only be contracted through tick bites is now outdated – deer and horse fly, as well as some mosquitos, can carry the bacteria too. Only about 50% of patients diagnosed with Lyme disease ever remember being bitten by a tick and only 10% have ever had an erythema migrans, also known as a bulls-eye rash, which is so often considered characteristic of Lyme disease.
The disease is not limited to rural locations and has been reported in urban areas including some London parks. The number of new cases each year in the UK is estimated to be as high as 15,000, and can in part be explained by a 73% increase in tick numbers in the UK in the last 10 years.
More controversially it has been suggested that Lyme disease can be transmitted in a number of other ways, including; blood transfusion, from mother to baby during pregnancy, and breastfeeding as well as through sexual intercourse. According to DR Ray Jones, an expert in paediatric tick-born diseases, congenitally acquired Lyme disease manifests in specific symptoms in children, ranging from frequent ear and throat infections and reflux to developmental delays and poor muscle tone (see diagram 1)
What are the key symptoms?
In the early stages of Lyme disease, it may feel like a very bad case of flu with high fever, headaches, nausea, chills, body aches and pains, and overwhelming fatigue. If Lyme disease goes untreated it can become something much more sinister.
Lyme disease is considered the “great imitator” as it can mimic so many other illnesses and uses molecular mimicry to evade the immune system. In paediatric cases, a host of symptoms can be expected, ranging from headaches and insomnia to outbursts and mood swings (see diagram 2). Children can’t always explain what feels wrong, especially when symptoms can vary in severity and come and go over time. Their bodies may hurt and they may feel overwhelmed with school-work or they may become severely sensitive to light and sound.
Lyme disease can affect any organ of the body (often multiple organs are affected), including the brain and nervous system – the Borrelia bacteria can be found within the central nervous system as early as twelve hours after entering the bloodstream.
Lyme disease and co-infections
Lyme disease doesn’t usually travel alone and can go hand in hand with a number of other co-infections. There appear to be some co-infections which are more commonly found in autism and include; Chlamydia Pneumonia, Mycoplasma, Bartonella, Coxsackie (very common), Epstein Barr Virus, and Cytomegalovirus. Diagram 3 outlines the key symptoms unique to each co-infection.
How should you test for Lyme disease?
Current standard testing for Lyme disease misses out over 50% of those affected. The two most commonly used tests are; enzyme-linked immunosorbent assay, known as ELISA, and the Western Blot test – these tests are simply not accurate enough – antibodies can take between 4 to 6 weeks to develop to detectable levels and can only be produced if the body has adequate “health” to produce antibodies – in many cases those suffering from Lyme disease have significant symptoms and health issues, and may not have the vitality to produce antibodies.
Armin laboratories in Germany, which specialize in Lyme and co-infection testing, claim to offer accuracy levels of over 90%. Having a negative blood test for Lyme disease does NOT mean that Lyme disease is not present, and needs to be considered based on the clinical picture.
Other common lab findings, which go hand in hand with Lyme disease are; abnormal lipid profile, insulin resistance, borderline low white blood cells, low thyroid function, low cortisol, DHEA and testosterone, and low alkaline phosphatase (although in children this last marker is less reliable).
SUMMARY
The neuropsychiatric manifestations of chronic Lyme disease and their possible connection to autism cannot be ignored. It took over 100 years for the medical profession to accept the connection between helicobacter pylori and stomach ulcers, with the first group of scientists being ridiculed and the last group of scientists being given the Nobel Prize for their “discovery”.
More good quality research is clearly needed into the connection between Lyme disease and autism spectrum conditions. This can take time – time that our children cannot afford. Investigating and treating chronic Lyme disease and co-infections, in autism should be considered if the clinical picture warrants it.


